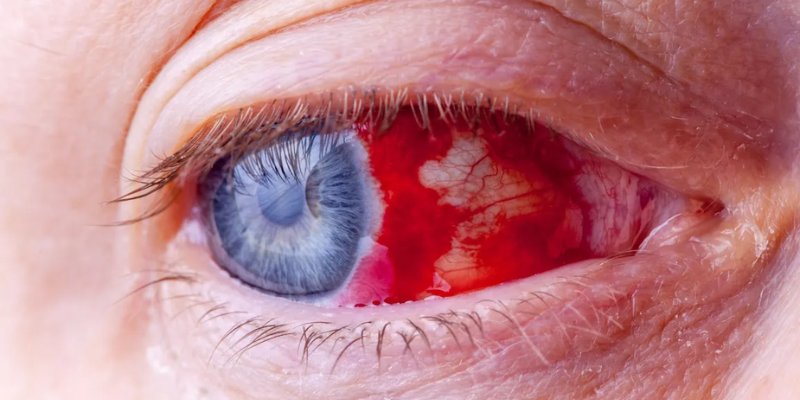
What Is Ocular Trauma?
Ocular trauma refers to any injury to the eye or its surrounding structures caused by mechanical, chemical, thermal, or radiation-related forces. Eye injuries can range from minor scratches to severe vision-threatening damage and require prompt evaluation and treatment to prevent permanent vision loss.
Causes & Risk Factors
Ocular trauma can occur due to :
- Workplace accidents — construction, factories, laboratories
- Sports injuries — balls, racquets, or physical contact
- Household accidents — chemicals, sharp objects, tools
- Road traffic accidents — blunt trauma or foreign bodies
- Assaults or fights — blunt or penetrating injuries
- Chemical or thermal burns — acids, alkalis, hot liquids, or flames
Risk factors include lack of protective eyewear, high-risk occupations, children, and elderly individuals.
Symptoms & Signs
The severity of symptoms depends on the type of trauma :
- Eye pain or discomfort
- Redness, swelling, or bruising around the eye
- Blurred or decreased vision
- Double vision or difficulty focusing
- Sensitivity to light (photophobia)
- Foreign body sensation
- Bleeding from the eye or eyelid
- Visible corneal or conjunctival damage
Diagnosis & Examination
Prompt assessment by an ophthalmologist is essential :
- Visual acuity testing to measure the impact on vision
- Slit-lamp examination to assess cornea, anterior chamber, lens, and conjunctiva
- Dilated fundus examination to check retina and optic nerve
- Imaging studies — X-ray, CT, or ultrasound if intraocular foreign bodies or orbital fractures are suspected
- Tear film and intraocular pressure assessment
Management Approaches
Emergency / Immediate Care
- Chemical injuries: Immediate irrigation to neutralize pH
- Foreign body removal: Superficial or intraocular foreign bodies carefully extracted
- Wound protection: Eye shield or patch to prevent further injury
- Pain management: Topical or systemic medications as required
- Tetanus prophylaxis if penetrating injuries are present
Surgical / Advanced Interventions
- Corneal or scleral repair for lacerations or perforations
- Lens extraction in traumatic cataract
- Vitrectomy for vitreous hemorrhage or retinal detachment
- Repair of orbital fractures if necessary
- Management of chemical burns including amniotic membrane transplantation or limbal stem cell transplantation (SLET) in severe cases
Risks & Complications :
- Permanent visual impairment or blindness
- Corneal scarring or opacity
- Retinal detachment or vitreous hemorrhage
- Secondary glaucoma
- Infection or endophthalmitis
- Diplopia (double vision) from muscle or orbital injury
Post-Treatment Care & Recovery
- Regular follow-up visits to monitor healing and visual function
- Use of prescribed eye drops and medications
- Avoidance of strenuous activity or trauma until cleared by the ophthalmologist
- Protective eyewear for ongoing prevention
- Rehabilitation for visual recovery, including low vision support if needed