What Is Corneal Transplantation?
Corneal transplantation, also known as keratoplasty, is a surgical procedure that replaces a damaged, scarred, or diseased cornea with healthy donor tissue. The cornea is the clear, dome-shaped surface at the front of the eye that helps focus light. When it becomes cloudy or irregular, vision is significantly impaired. Corneal transplantation restores transparency, improves vision, relieves pain, and enhances quality of life.
Conditions That May Require Corneal Transplant
- Pseudophakic bullous keratopathy (Corneal oedema post cataract surgery)
- Keratoconus (progressive thinning and bulging of the cornea)
- Corneal scarring due to infections, injuries, or previous surgery
- Fuchs’ endothelial dystrophy (corneal cell loss causing swelling and vision loss)
- Corneal edema (persistent swelling not responsive to medication)
- Thinning, perforation, or trauma-related corneal damage
- Failed previous corneal transplant
- Hereditary corneal disorders
Symptoms Indicating Need for Transplant
- Blurred or cloudy vision not correctable with glasses or lenses
- Severe eye pain from corneal swelling or surface irregularities
- Glare, halos, or distortion of vision
- Recurrent corneal infections
- Vision loss impacting daily activities
Types of Corneal Transplantation
Modern corneal surgery is customized to the patient’s condition :
Penetrating Keratoplasty (PK)
Full-thickness corneal transplant, replacing all layers of the cornea.
Endothelial Keratoplasty (DSEK / DMEK)
Partial-thickness transplant replacing only the diseased innermost endothelial layer, leaving the rest of the cornea intact.
Deep Anterior Lamellar Keratoplasty (DALK)
Removes and replaces the front layers of the cornea while preserving the healthy endothelium.
Artificial Corneal Implants (Keratoprosthesis)
Used in rare cases where traditional transplantation is not possible.
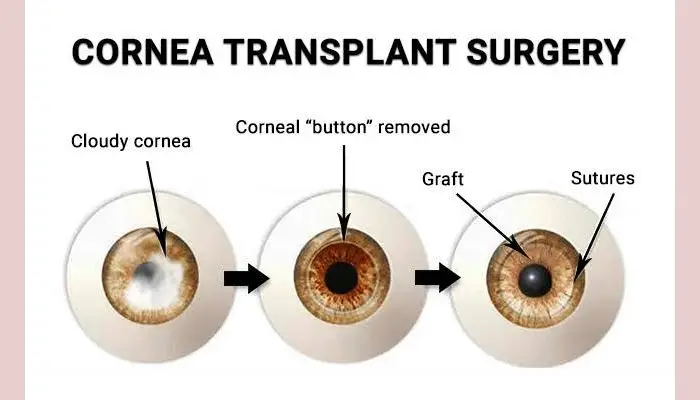
Surgical Procedure
- Detailed preoperative eye examination and corneal measurements
- Selection of suitable donor corneal tissue from an eye bank
- Local or general anesthesia depending on patient needs
- Removal of the diseased portion of the cornea
- Placement and suturing (or layering) of donor tissue
- Application of protective eye shield and medications for healing
Risks & Complications
Although highly successful, corneal transplantation carries certain risks :
- Graft rejection (immune response against donor tissue)
- Infection
- Astigmatism or irregular corneal shape
- Recurrence of original disease in some cases
- Detachment of graft layers (in partial transplants)
- Glaucoma or increased eye pressure
- Need for repeat transplant in rare cases
Postoperative Care & Recovery
- Use of prescribed eye drops (antibiotics, steroids, lubricants)
- Protective eyewear to avoid accidental injury
- Avoidance of rubbing or pressing the eye
- Regular follow-up visits to monitor healing and graft clarity
- Stitches may remain for months; some are removed gradually
- Vision recovery may take several months to stabilize
- Long-term monitoring for signs of rejection (redness, pain, blurred vision, sensitivity to light)